The Spine Volumetric BMD Advantage
QCT's ability to assess trabecular, volumetric mineral density, independent of cortical bone, has long been recognized as advantageous because of the high metabolic activity of trabecular bone relative to cortical bone.
Less commonly recognized is that volumetric mineral density measurements circumvent a number of factors that confound DXA area density measurements at the spine.
Common DXA-spine confounding factors include:
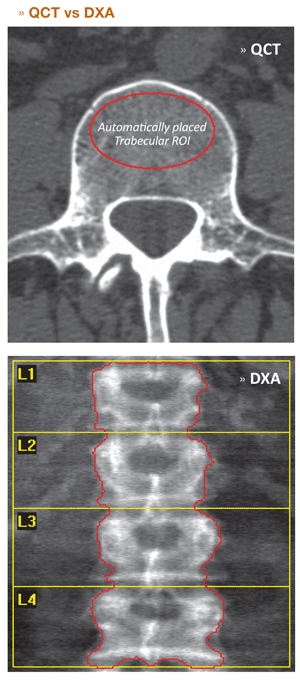
- The majority of mineral mass as measured by DXA at the spine is attributable to mineral mass in the posterior elements.
- Area density estimates increase as vertebral disc spaces narrow and/or vertebral heights decrease.
- Area density estimates increase as a result of osteophytosis associated with conditions such as osteoarthritis.
- Area density estimates increase as a result of aortic calcifications and other extraosseous sources of mineral.
Collectively these factors degrade sensitivity and specificity when DXA is used to identify individuals at increased risk of fracture and assess the efficacy of treatments intended to reduce fracture risk.
By virtue of the anatomical detail intrinsic to CT images, QCT can be used to characterize metabolically important, trabecular bone in regions unaffected by common degenerative changes at the spine and aortic calcifications, and exclusive of cortical bone.
55% to 90% of osteoporosis-related fractures occur in individuals that would not be diagnosed with osteoporosis based on a DXA BMD test.*
The 3D Imaging Advantage
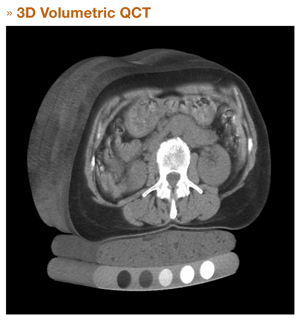
While conventional QCT relies upon single, thick CT images through each of multiple vertebrae, 3D QCT exploits CT's ability to construct a three dimensional representation of human anatomy using many thin images.
This results in a number of technical and clinical advantages, including:
- Ability to assess BMD in patients with scoliosis or other complex spinal deformities.
- Improved measurement precision because of decreased reliance upon the skill of a CT operator to precisely position a single, thick slice through a vertebra.
- Shortened scan times due to elimination of CT gantry tilt
- Support for modern multi-slice CT scanners which no longer support gantry tilt.
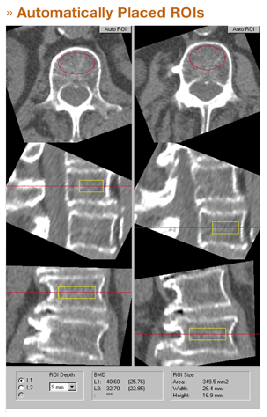
Faster, Easier
- Define only start and end points.
- No gantry tilt, no scan pauses.
- Helical/multi-slice scan in seconds.
- Scan only 2 instead of 3 or 4 vertebra.
- Combine spine and hip in one fast scan.
* Stone, et al; 2003; J Bone and Mineral Research.

